This becomes particularly important in the critically ill patient and has an increased benefit the further the patient needs to travel. Decreased transport time: Total time to patient arrival may not actually be shorter (due to travel to airport or helipad, or collection of crew members, equipment or blood products from a facility), the amount of time the patient spends in transit is decreased due to increased speeds of air transport.By comparison, ground transport crews typically are designated basic life support (BLS), advanced life support (ALS) or critical care (CC) capable. This definition is broad and in addition to EKG interpretation, pacing, defibrillation, intubation, cricothyrotomy, and needle thoracostomy may include titration of drips, ventilator management, pericardiocentesis, umbilical vein catheterization, etc. Therefore, aeromedical crews must provide critical care – care that exceeds the scope of a paramedic as defined by the National Highway Traffic Safety Administration’s (NHTSA) National EMS Scope of Practice Model. Provide critical care: Candidates for aeromedical transport are critically-ill medical or trauma patients requiring tertiary or specialty services not immediately available in their region and are often at risk of decompensation.In addition to a pilot, the crew usually consists of at least two members and may be any combination of the following:Ĭourtesy of Tim Snopek, used with permission by Flight for Life Emergency Medical Air Transport. There are no universal regulations regarding crew composition and this varies between region and EMS system. However, there may be a higher level of direct or on-line medical control amongst aeromedical services where the medical staff speak directly with a physician providing medical direction. Like any EMS system, aeromedical crew operate under indirect medical control using protocols and standing orders. Therefore, they must be familiar with aircraft safety and be able to function within various transport vehicles in their system. In addition, crew may be responsible for ground transport (ambulance) to and from the hospital, airport or helipad. 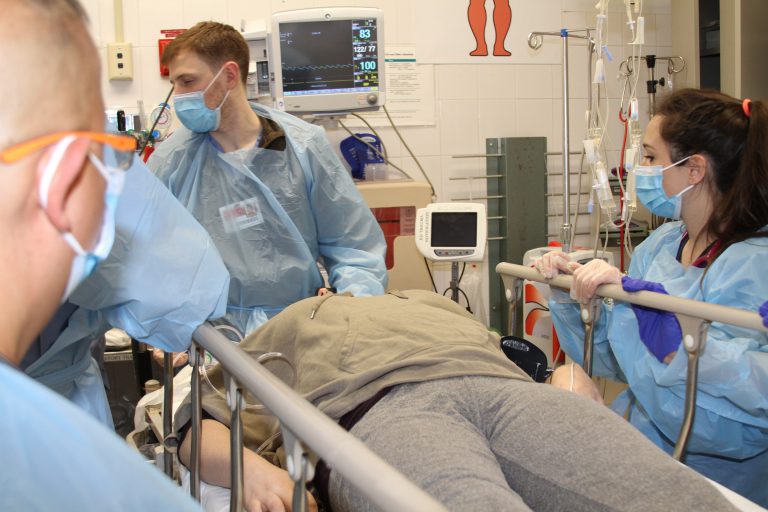
Therefore a basic understanding of aeromedical systems, patient selection and flight physiology is imperative.Īeromedical transport systems may include rotary wing (helicopter) or fixed-wing (airplane) aircraft. Certain patient populations may specifically benefit from aeromedical transport, and determining which patients are appropriate for transport is often the responsibility of the emergency physician (EP). The time-sensitive nature and high level of care required by these patients make aeromedical services a key component of emergency medicine and Emergency Medical Services (EMS). Prehospital and interhospital transport of critically ill patients play an important role in providing access to tertiary and specialty care facilities. Identify safety themes pertinent to aeromedical transport.Understand the roles of the transferring physician and AEMS crew in aeromedical transport.Understand how basic concepts of flight physiology may impact care.Determine patients who may benefit from aeromedical transport.Recognize the advantages and disadvantages of aeromedical services.Describe the structure of an aeromedical emergency medical services (AEMS) system.SAEMF/CDEM Innovations in Undergraduate Emergency Medicine Education GrantĬareer Development and Mentorship CommitteeĬDEM Medical Education Fellow Travel ScholarshipĪuthor: Jamie Aranda, MD, Medical College of WisconsinĮditor: Jonathan Fisher, MD, Maricopa Medical Center Virtual Rotation and Educational ResourcesĮMF/SAEMF Medical Student Research Training Grant Visit us on Twitter LinkedIn Facebook YouTube Instagram
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
